In 2020, oesophageal cancer was the sixth most common cause of cancer death worldwide, the seventh most common cancer in men and the 13th most common cancer in women. In the same year, Singapore reported 234 new cases of oesophageal cancers, and of these, 220 patients could not have treatment and died of the cancer it had already spread.
However, oesophageal cancer is curable if detected and treated promptly and aggressively at an early stage. Learn more about oesophageal cancer, signs to look out for, treatment and prevention methods.

Oesophageal cancer, like many other cancers, is categorised into stages. The stages of oesophageal cancer are typically defined by the TNM system, which takes into account the size and extent of the primary tumor (T), the involvement of nearby lymph nodes (N), and the presence of distant spread to different organs – metastasis (M). Here, we outline the stages and what they mean:
At this early stage, abnormal cells are found only in the innermost layer of the oesophagus lining, without penetrating deeper layers. It is often referred to as “high-grade dysplasia” or “in situ” cancer. Treatment at this stage is highly effective, often involving endoscopic procedures to remove or destroy the abnormal cells.
In Stage I, the cancer has invaded the deeper layers of the oesophagus but it has not spread to lymph nodes or distant sites. The tumor is relatively small and confined to the oesophagus. Surgery or endoscopic therapy is a common treatment approach for Stage I oesophageal cancer.
In this stage, the tumor has grown deeper into the wall of the oesophagus and it may have spread to the the nearby lymph nodes. Surgical resection is often recommended. Depending on the histology of the cancer that is removed, chemotherapy and/or radiation therapy may also need to be given.
Oesophageal cancer in Stage III has spread further into the surrounding tissues, possibly affecting nearby structures, such as the airways or blood vessels. Lymph nodes are often involved. Treatment usually involves a combination of surgery, chemotherapy, and radiation therapy.
At this advanced stage, the cancer has spread to distant organs or lymph nodes, such as the lungs, liver, or distant lymph nodes. Stage IV oesophageal cancer is considered incurable, and the focus is on palliative care to manage symptoms and improve the patient’s quality of life. Treatments may include chemotherapy, targeted therapy, immunotherapy, and radiation therapy to alleviate symptoms and slow disease progression.
Sometimes, oesophageal cancer may come back after initial treatment. The recurrence can occur locally (in the oesophagus or nearby tissues) or distantly (in distant organs or lymph nodes). Treatment for recurrent cancer depends on the location and extent of the recurrence and the patient’s overall health.
We all do suffer with occasional heartburn every few weeks (2-3 times) depending on what we eat and on our stress levels. However, when this becomes more frequent it may my be the early signs of esophageal cancer.
One of the early signs of oesophageal cancer is difficulty or pain while swallowing (dysphagia).
Rapid and unintentional weight loss can be indicative of a more advanced stage of the disease.
Long-term and severe acid reflux can lead to Barrett’s oesophagus, a precursor to adenocarcinoma.
Oesophageal cancer may cause chest pain or discomfort, especially when swallowing.
A persistent cough or hoarseness may be a symptom, as the tumour can affect the nearby airways.
Frequent vomiting and regurgitation may occur, sometimes containing blood.
A Gastroscopy is a minimally invasive procedure in which a flexible, lighted tube with a camera at the tip (endoscope) is inserted through the mouth and into the oesophagus. This allows the oesophageal cancer surgeon to directly visualise the lining of the oesophagus and obtain tissue samples (biopsies) for further examination. It is a quick and painless procedure undertaken with a light sedation
When you are confirmed with oesophageal cancer, advanced imaging techniques, such as CT scans, PET scans, and MRI scans, are commonly used to determine the extent and stage of oesophageal cancer if needed. These tests provide detailed images of the oesophagus and surrounding structures, helping doctors plan the most appropriate treatment strategy.
Biopsy samples obtained during endoscopy are sent to a pathology laboratory for analysis. Pathologists examine the tissue samples under a microscope to confirm the presence of cancer, determine the cancer type (e.g., squamous cell carcinoma or adenocarcinoma), and assess the cancer’s aggressiveness. This information is crucial in tailoring the treatment plan.
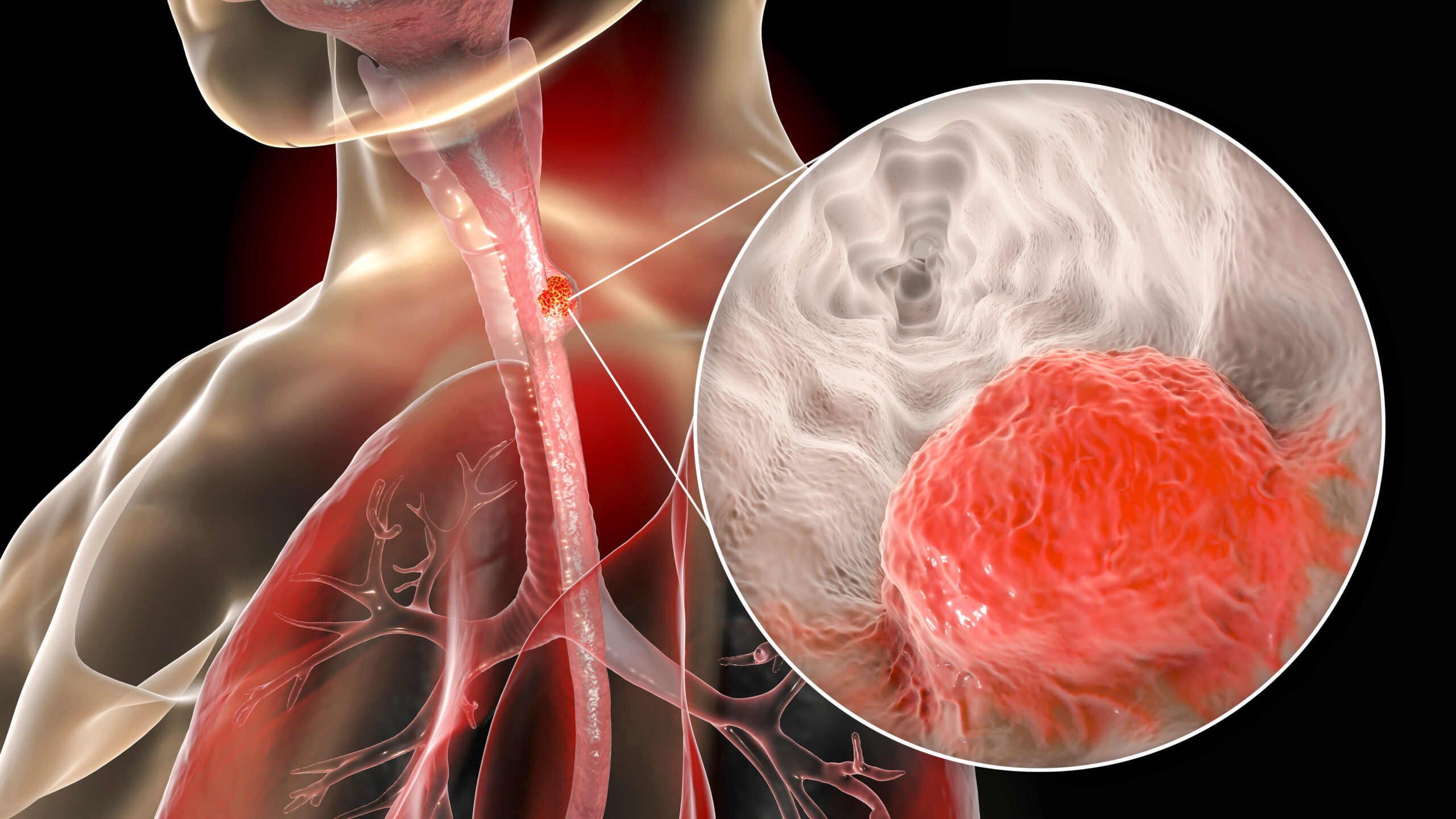
Treatment for oesophageal cancer varies depending on the stage and type of cancer, as well as the patient’s overall health. Common treatment modalities include:
Endoscopic treatments, such as endoscopic mucosal resection (EMR) or endoscopic submucosal dissection (ESD), are used for early-stage oesophageal cancers, especially in cases of dysplasia or carcinoma in situ. A flexible tube with a camera and specialised tools is inserted through the mouth to remove or destroy cancerous tissue, often avoiding the need for open surgery.
Traditional open surgery involves making a large incision in the chest or abdomen to access and removing the oesophagus with the cancer. The stomach is then used to connect the intestines back to the remaining oesophagus. Minimally invasive surgical techniques are increasingly preferred when possible due to faster recovery and reduced post-operative pain.
Laparoscopic surgery, also known as minimally invasive surgery, involves making several very small incisions and using a camera with specialised instruments to remove the oesophagus and cancer. This approach typically results in quicker recovery, shorter hospital stays, less complications and faster recovery times compared to open surgery.
Radiation therapy uses high-energy rays to target and kill cancer cells or shrink tumors. It can be administered externally (external beam radiation) or internally (brachytherapy). In oesophageal cancer, radiation therapy is often used in combination with other treatments, such as chemotherapy, before surgery to shrink the tumor or after surgery to kill any remaining cancer cells. It can also help alleviate symptoms in advanced cases, such as difficulty swallowing.
Chemotherapy involves the use of drugs to kill rapidly dividing cancer cells. It is commonly used in oesophageal cancer, either before surgery (neoadjuvant chemotherapy) or after surgery (adjuvant chemotherapy) to reduce the risk of recurrence depending on the stage of the cancer. It can also be used in combination with radiation therapy (chemoradiation) for locally advanced disease. In advanced or metastatic cases, chemotherapy can help control the cancer and relieve symptoms.
Targeted therapy drugs are designed to target specific molecules or pathways involved in the growth and spread of cancer cells. They are often used in cases of advanced oesophageal adenocarcinoma that may not respond well to traditional chemotherapy. Targeted therapy can use drugs that inhibit proteins like HER2 or VEGF, which are often overexpressed in certain oesophageal cancers and so helps destroy the cancer cell.
Immunotherapy is an innovative approach that stimulates the patient’s immune system to recognize and attack cancer cells. Immune checkpoint inhibitors have shown promise in the treatment of advanced oesophageal cancer, particularly in patients whose cancer has progressed despite other treatments. It has help to increase the remain life span in these patients.
Palliative care is an essential component of oesophageal cancer treatment, particularly in advanced cases. It focuses on managing symptoms, providing pain relief, and improving the patient’s quality of life. Palliative care specialists work in conjunction with surgical oncologist to address the physical, emotional, and psychosocial aspects of cancer care. The choice of treatment depends on the specific circumstances of the patient, the type and stage of cancer, and the patient’s overall health.
Oesophageal cancer is more common in older adults, with the risk increasing significantly after the age of 55.
Men are more likely to develop oesophageal cancer than women.
Smoking and heavy alcohol consumption are among the most significant risk factors. The combination of smoking and drinking alcohol increases the risk even further.
Persistent and severe acid reflux can lead to Barrett’s oesophagus, a condition that increases the risk of oesophageal adenocarcinoma.
Excess body weight, especially when it accumulates around the abdomen, is a risk factor for oesophageal adenocarcinoma.
Diets low in fruits and vegetables and high in processed or red meats have been associated with an increased risk of oesophageal cancer.
A family history of oesophageal cancer may raise an individual’s risk, although the genetic factors involved are not yet well understood. Certain regions of the world have a high rate of esophageal cancer.
Oesophageal cancer risk factors can vary based on the type of oesophageal cancer (squamous cell carcinoma or adenocarcinoma) and geographic region, as certain risk factors are more prevalent in specific areas. Here are some common risk factors associated with oesophageal cancer:

While some risk factors for oesophageal cancer, such as age and gender, cannot be changed, there are several ways to reduce your
Smoking is a significant risk factor for oesophageal cancer. Quitting can lower your risk.
Excessive alcohol consumption is linked to an increased risk of oesophageal cancer. Drinking in moderation or abstinence is advisable.
If you have chronic heartburn, seek medical treatment and assesment to prevent the development of Barrett’s oesophagus.
A diet rich in fresh fruits and vegetables may help lower your risk. Avoiding excessive consumption of processed foods and red meat is also recommended.
Staying physically active can contribute to overall health and may lower cancer risk.
If you have risk factors such as a family history of oesophageal cancer, consult with a healthcare provider about screening and surveillance options.
Oesophageal cancer is a serious condition, but with early detection and appropriate treatment, it can be managed effectively. Understanding the symptoms, treatment options, and preventive measures is essential in reducing the impact of this disease on individuals and their families. It’s important to note that many early symptoms, such as persistent indigestion or difficulty swallowing, can also be signs of stomach cancer, making prompt medical evaluation crucial for both conditions Regular check-ups and a healthy lifestyle are your best defenses against oesophageal cancer. If you suspect any symptoms or have concerns, don’t hesitate to seek medical advice from a healthcare professional.
A series of tests to confirm your diagnosis and determine the stage of your cancer.
Our multi-disciplinary team will work with you to create a personalized treatment plan.
This may involve surgery, chemotherapy, radiation therapy, or a combination of treatments.
After treatment, we will focus on your recovery, including nutritional support and physical therapy.
Regular check-ups and imaging to monitor your health and watch for any signs of recurrence.
We understand that navigating the financial aspects of cancer treatment can be stressful. Our team is here to help you understand your insurance coverage and the costs associated with your treatment. We are accredited to work with a wide range of insurance providers. Please contact our clinic for more information.
The most common symptom is difficulty swallowing (dysphagia). Other symptoms include unexplained weight loss, chest pain, and a persistent cough or hoarseness.
Diagnosis is typically made through an endoscopy, where a thin, flexible tube with a camera is used to examine the oesophagus and take a tissue sample (biopsy).
You will likely have a feeding tube for a period after surgery. Our team, including a dietitian, will work with you to gradually reintroduce food and develop a long-term nutrition plan.